
As a genetic condition, the syndrome is ultimately caused by changes to a person's DNA, known as genetic mutations. The individual heart muscle cells communicate with each other with electrical signals that are disrupted in those with Brugada syndrome. Sodium channel blocking medications, commonly used to treat cardiac arrhythmia, may also worsen the tendency to abnormal heart rhythms in patients with Brugada syndrome and should be avoided. Abnormal heart rhythms may also occur during fever or following excessive alcohol. These situations are linked to periods when the vagus nerve is activated, referred to as periods of high vagal tone. The abnormal heart rhythms seen in Brugada syndrome often occur at rest, following a heavy meal, or even during sleep. However, blackouts can occur in those with Brugada syndrome despite a normal heart rhythm due to a sudden drop in blood pressure, known as vasovagal syncope. If a dangerous heart rhythm does not stop by itself and is left untreated, the person may have a fatal cardiac arrest. Blackouts may be caused by brief abnormal heart rhythms that revert to a normal rhythm spontaneously. While many of those with Brugada syndrome do not have any symptoms, Brugada syndrome may cause fainting or sudden cardiac death due to serious abnormal heart rhythms such as ventricular fibrillation or polymorphic ventricular tachycardia. Chen first described the genetic abnormality of SCN5A channels It was firstly described by Andrea Nava and Bortolo Martini in Padova in 1989 but it is named after the Catalan cardiologists Pedro and Josep Brugada who described the condition in 1992. The onset of symptoms is usually in adulthood. It is more common in males than females and in those of Asian descent. The condition affects between 1 and 30 per 10,000 people. 
Testing people's family members may be recommended. Isoproterenol may be used in the short term for those who have frequent life-threatening abnormal heart rhythms, while quinidine may be used longer term. In those without symptoms the risk of death is much lower, and how to treat this group is less clear. Those at higher risk of sudden cardiac death may be treated using an implantable cardioverter defibrillator (ICD). Similar ECG patterns may be seen in certain electrolyte disturbances or when the blood supply to the heart has been reduced. Medications such as ajmaline may be used to reveal the ECG changes. Diagnosis is typically by electrocardiogram (ECG), however, the abnormalities may not be consistently present. The most commonly involved gene is SCN5A which encodes the cardiac sodium channel. Some cases may be due to a new genetic mutation or certain medications. Ībout a quarter of those with Brugada syndrome have a family member who also has the condition. The abnormal heart rhythms seen in those with Brugada syndrome often occur at rest. Those affected may have episodes of syncope. It increases the risk of abnormal heart rhythms and sudden cardiac death. Watchful waiting, implantable cardioverter defibrillator (ICD) īrugada syndrome ( BrS) is a genetic disorder in which the electrical activity of the heart is abnormal due to channelopathy. Romano-Ward syndrome, arrhythmogenic cardiomyopathy, Duchenne muscular dystrophy Typical type 1 ECG changes seen in Brugada syndromeįamily history, Asian descent, male Įlectrocardiogram (ECG), genetic testing Sudden unexplained nocturnal death syndrome, bangungut, pokkuri death syndrome
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
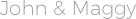
 RSS Feed
RSS Feed
